|
Gulani believes transplants should be the last option for keratoconus patients because not only are they an interventional surgery that involves donor tissue (that can be rejected), but also because it doesn’t lead to vision with freedom from contact lenses or glasses.ĭr. This is analogous to putting cement on a bent back (scoliosis) with a promise of preventing further bends in a spine, but why wouldn’t a doctor straighten the spine (keratoconus) first?Īs a renowned corneal transplant surgeon himself, Dr. Gulani does offer it as an important ingredient in the spectrum of keratoconus treatments, but most eye doctors are indiscriminately cross-linking every keratoconus patient with a promise of preventing worsening. With nearly three decades of experience with cross-linking technologies all over the world, Dr. Though we cannot guarantee outcomes in such complex Keratoconus cases, 1000’s of patients have shared their testimonials and stories (with no incentive) on our website with a desire to spread hope among fellow patients and possibly inspire their eye surgeons to perform. Gulani, who teaches worldwide to encourage every ophthalmologist (eye surgeon), optometrist, and all levels of eye care providers to fight for their patients’ vision. “ A doctor’s inability should never become the patient’s disability,” says Dr. 
Often, telling patients to “live with it” or providing less than optimal options. Most patients travel to us desperate for help having been denied opportunities by their eye doctors and surgeons who have assumed their own inability or the patient’s lack of potential to see. 
Additionally, many patients may develop a condition called Lasik ectasia (cone-like bulging of the cornea similar to keratoconus) as a complication of LASIK surgery. It is also important to know that many patients may actually not complain of any symptoms at all while looking for options of LASIK surgery until sophisticated diagnostic technologies at our Institute detect keratoconus at its earliest stages so we can promptly tailor the treatment path of such patients. We look forward to helping you.Having seen a wide variety of Keratoconus patients from all over the world, the most common symptoms they have, despite their unique situations, include: blurred vision, halos around lights, starbursts, double or distorted vision, difficulty driving at night, and vision fatigue. If you have been diagnosed with keratoconus or pellucid marginal degeneration and would like to schedule a consultation, please use our online appointment request or call 33. Have you been diagnosed with Keratoconus or PMD? In addition, he uses only the best equipment on the market to successfully treat these eye conditions. Jon Scott is an expert in diagnosing and treating Keratoconus and PMD. 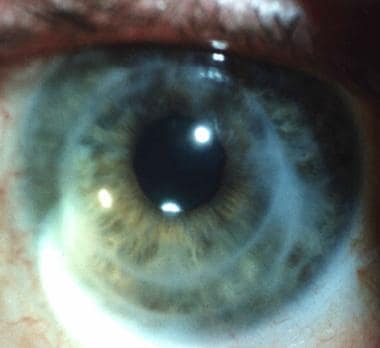
Once again, highly specialized contact lenses can be used to treat these disorders.ĭr. While some of these patients actually had undiagnosed keratoconus or pellucid marginal degeneration prior to surgery, many cases are thought to be caused by the biomechanical effects of the surgery. While the majority of patients can be treated with contact lenses, in severe cases, both disorders can lead to the need for a corneal transplant.Įven in the hands of the most skilled physicians, ectasia can be induced by refractive surgery (LASIK, PRK, RK, etc.). While this doesn’t correct or reverse the condition it has been shown to significantly strengthen the cornea to keep it from getting worse. It involves placing vitamin-A drops in the eye and exposing it to a certain wavelength of ultraviolet light. FDA trials are currently underway for a procedure called corneal cross-linking.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
